HIPEC
Warm chemo inside the belly - called HIPEC - is a precise method for certain cancers spreading in the abdominal space. Surgery clears big tumors first, then liquid medicine, warmed just right, flows in to catch what's left behind. Not every patient fits this path; only specific cases benefit when stray cells hide after cutting. Years of practice show it can touch spots regular treatments miss. Heat helps the drug work deeper, staying focused where it matters most.
Inside the belly space sit key body parts like the stomach, gut loops, liver, spleen, along with sex-related structures, each covered by a delicate wrap called the peritoneum. When certain cancers move across this layer, doctors call it peritoneal surface disease. Tumors starting in the appendix, large intestine, ovaries, or belly organ sometimes behave this way, just like uncommon growths deep inside. If cancer lands on those inner linings, standard drug treatments given through veins usually struggle to reach them well. To handle that gap, specialists began using heated chemo fluid right at the site where bad cells hide.
From the start, patients undergo an extensive operation known as cytoreductive surgery. Inside the belly area, medical teams inspect closely, taking out any tumors they can see. Depending on how far things have spread, parts might come away - like sections of intestine or other involved areas, even the abdominal lining. Only tiny traces should stay behind after cutting, since that sets up the next phase well. Heat-based therapy later targets what's left at a cellular level.
After taking out the tumor, things move to the next step. This part uses a chemo mix warmed carefully - most times it sits at 41 to 43°C - and flows through the belly space for about 60 to 90 minutes. Because it’s warm, the medicine works better; heat helps it get deeper into tissue while also damaging cancer cells more fully.
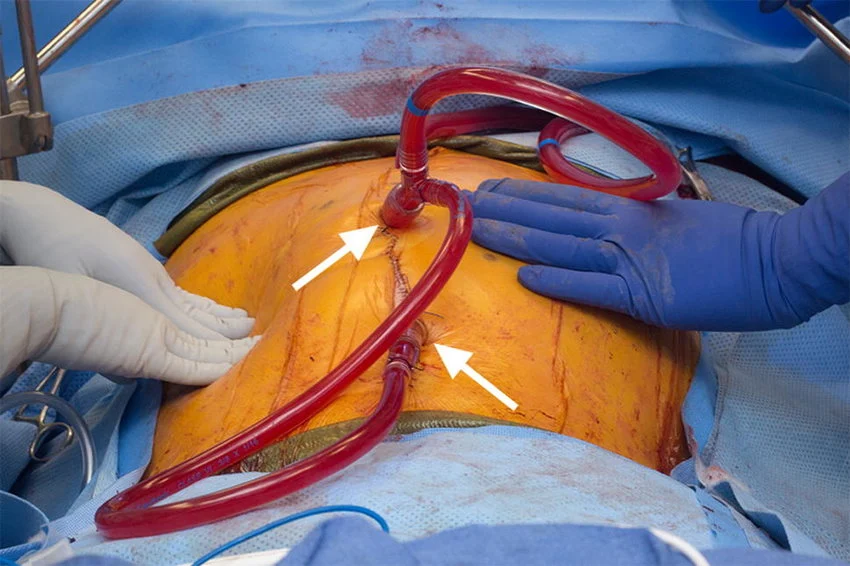
Now flowing through a custom loop, the chemo liquid moves steadily inside the belly space thanks to precise equipment. Throughout, medical staff watch heat levels, movement of fluid, and how the person is holding up - each detail matters. Once finished, out goes the medicine, then the team wraps up the operation.
What makes HIPEC stand out is how the chemo stays mostly where it's needed - within the belly area - instead of spreading through the bloodstream like regular IV treatments do. Higher doses can work right at the tumor site because of this setup, yet the rest of the body feels fewer harsh impacts tied to typical chemo. Since the medicine focuses so closely, organs and tissues beyond the abdomen aren’t hit as hard by the drugs.
Not everyone with belly cancer can get HIPEC. Before deciding, a close look at the person’s health matters most. The kind of cancer plays a role, also how far it has moved through the body. A doctor checks strength, eating habits, plus if organs like liver or kidneys work well. Getting rid of all tumors - or almost all - must seem doable. Scans give clues, blood tests add detail, and several specialists often weigh in together. Only then does the team decide if this approach fits.
Might take longer to bounce back from HIPEC compared to standard cancer operations since it mixes extensive belly surgery with strong chemo doses. Staying in the hospital under watch becomes normal afterward, along with help controlling discomfort and getting enough nutrients while slowly starting to move again. Digestive rhythms might shift at first, energy often dips, fluids redistribute inside the body, hurdles pop up early on in healing. Each person's path through this stage carries its own rhythm and timeline.
Success rides on how well the team works together - surgeons, anesthetists, ICU doctors, cancer specialists, nurses - all skilled in their roles. Timing must be sharp; even small delays matter. Precision shapes every move during surgery. Recovery afterward needs high-level medical backing.
Some people find real gains through HIPEC, particularly when standard treatments fall short. When the right candidates are picked, certain cancer types respond with longer survival. A careful match between patient and procedure makes a difference others can’t always offer.
Now shaping how cancer care moves forward, HIPEC shows medicine's shift to precision. Not one-size-fits-all anymore, today’s methods respond to where tumors grow, how they travel, what drives them - each factor guiding better results.
What happens before surgery matters just as much as the operation. Good nutrition helps the body cope, while stopping infections early makes a big difference. Support with feelings and mindset plays a role too, alongside clear plans for healing afterward. When someone has had cancer treatments in the past, fitting everything to their specific needs gains greater weight. How people handle HIPEC ties closely to these behind-the-scenes steps.
Checking in after HIPEC still matters. Even when things seem stable, scans keep happening along with blood tests and visits to the cancer specialist - this combo helps catch changes fast. How the tissue looks under the microscope can shift what comes next. Some people end up needing more medicine through the veins based on those results.
Inside the belly, some people get a unique kind of help through HIPEC. This method pairs exact surgical work with strong medicine aimed right where it's needed. Not everyone qualifies, yet for certain situations it has changed outcomes dramatically. Few treatments have made such a difference when targeting cancers tucked deep within the abdomen.